I wanted to shed some light on the role of stress and sleep in Hashimoto’s. We know that stress is never helpful, right? One of the earliest cases of thyroid disease was actually connected to a woman who was thrown down a flight of stairs in a wheelchair — how’s that for stressful!
Over the past few years, I’ve worked with over a thousand people with Hashimoto’s, and have found that most cases of Hashimoto’s involve high stress levels. With Hashimoto’s (and even without), stress and sleep deprivation go hand-in-hand.
Most of us understand sleep deprivation as a simple lack of sleep. But the truth is that while you may be sleep deprived simply because of the quantity of your sleep, or because you’re not sleeping enough, you may also be sleep deprived because of the quality of your sleep. Some of us may be getting a full-night’s sleep hours-wise, but may still wake up unrested, or find ourselves unusually tired throughout the day.
One common condition behind poor sleep quality is a condition known as sleep apnea.
In this article, you’ll learn:
- How sleep quality affects Hashimoto’s
- What sleep apnea is
- Symptoms and risk factors of sleep apnea
- How to test for sleep apnea
- Conventional and root cause approaches to improving sleep apnea
The Link Between Sleep Deprivation and Adrenal Fatigue
Sleep deprivation and adrenal fatigue are closely linked to the hypothalamic-pituitary-adrenal (HPA) axis.
The HPA axis is an intricate system of direct and indirect feedback mechanisms that regulate the body’s reaction to stress. It plays a role in regulating multiple systems in our bodies, including:
- The immune system
- The digestive system
- Our moods
- Our metabolic processes
- Our libido
When the body experiences stress, various hormones can become unbalanced, and this puts stress on the HPA axis.
When our HPA axis is stressed and not working properly, this can lead to symptoms like fatigue, poor immune function, blood sugar imbalances, inflammation, and irritability — collectively known in alternative medicine circles as “adrenal fatigue.”
Most people with Hashimoto’s have some degree of adrenal fatigue (in fact, 90 percent of those I have tested, do); and in my survey of 2000+ people with Hashimoto’s, “a lack of sleep” is the most frequently cited reason why people with Hashimoto’s feel worse. As mentioned above, this could actually be due to having poor quality sleep.
When we have a poor quality of sleep, it just puts more stress on the HPA axis. (Sleep deprivation is such a powerful stressor for the HPA axis that it’s what scientists use to induce HPA axis dysfunction in laboratory animals!)
And, as we know, adrenal fatigue and a stressed HPA axis can exacerbate Hashimoto’s. As such, it’s important to address the root cause of one’s sleep issues, which can sometimes be caused by sleep apnea.
What Is Sleep Apnea?
Sleep apnea is a chronic health condition that has been associated with low-grade inflammation in the body and is characterized by pauses in breathing while one is sleeping. As these pauses in breathing and lack of oxygen wake people up intermittently throughout the night (though they don’t usually remember it), the result is often un-refreshing, fragmented sleep despite sleeping longer than usual.
There are three types of sleep apnea:
- Central sleep apnea (CSA): In CSA, the person stops breathing due to “forgetting” to breathe, or due to a lack of effort in breathing. The “forgetting” to breathe or lack of effort in breathing, is due to the brain not sending the required signals to the muscles that control breathing.
- Obstructive sleep apnea (OSA): In OSA, the muscles at the back of the throat relax too much, leading to repeated upper airway obstructions. As such, an individual may stop breathing. This is the most common type of sleep apnea and is often associated with a significant reduction in blood oxygen saturation (due to the repeated obstructions). Additionally, OSA can lead to oxidative stress, which results in damage to the mitochondria (a component inside cells mainly known for its role in energy production). This type of sleep apnea is usually more common in individuals with Hashimoto’s — one 2012 study investigating OSA and Hashimoto’s, reported that approximately 47 percent of individuals with OSA also had Hashimoto’s thyroiditis.
- A mixed variation of CSA and OSA: This type includes elements of both types of sleep apnea — the interruption in breathing happens because of a blockage of airflow. However, a CPAP machine would not fully resolve the sleep apnea.
Symptoms of Sleep Apnea
The classical symptoms of sleep apnea include snoring, difficulty in waking up, restless sleep, nightmares about difficulty breathing, nasal speech, mouth breathing, attention deficit disorder (especially in children), fatigue and/or daytime sleepiness, and nasal congestion. Please note, not all of these need to be present for a person to have sleep apnea.
Furthermore, a scalloped tongue, which is often seen in thyroid disease, has also been correlated with sleep apnea.
People with sleep apnea may also test positive for thyroid antibodies (more on that in a minute).
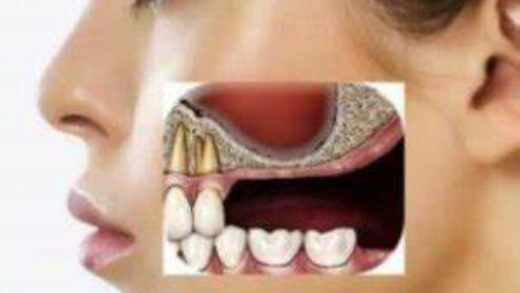
What is a Scalloped Tongue?
A scalloped tongue happens when a person’s tongue is too big for their mouth and spends too much time resting against one’s teeth. The scalloped tongue has ridges and wavy edges around its borders, and is frequently seen in those with Hashimoto’s and hypothyroidism.
In a 2005 study, Weiss and colleagues were able to compare the rates of sleep apnea and scalloped tongue. They found that 70 percent of people with sleep apnea had tongue scalloping, while only one person of the seven people in the control group (without sleep apnea), had a scalloped tongue. Furthermore, on a scale of scalloping from 0-3, with 3 being the most severe, the person without sleep apnea had a scalloping rating of 1, the lowest of the ratings. The researchers did not specify whether the higher degree of scalloping was predictive of higher rates of sleep apnea, but I would encourage anyone with a scalloped tongue to get checked out.
People who snore at night and/or have a scalloped tongue, should be suspected to have sleep apnea until proven otherwise! (I’ll talk about testing options in a minute.)
Nightmares in Sleep Apnea
Individuals who have sleep apnea have more emotionally negative dreams, or nightmares, than those who do not have sleep apnea. In particular, these nightmares often involve some sort of difficulty with breathing — some examples include choking, trying to breathe while underwater or in space, being strangled, or being stuck in an elevator.
Such nightmares can point to an individual having sleep apnea (if they were previously unaware or undiagnosed).
Who’s at Risk?
Sleep apnea affects about 2-9 percent of women and as many as 24 percent of men… but research suggests that 25-66 percent of people with Hashimoto’s also have sleep apnea!
Risk factors for sleep apnea include obesity, enlarged tonsils, enlarged tongue, having a small jaw (I find the work of Weston Price on this topic fascinating, if you ever want to learn more), allergies, sinus problems, a deviated septum, and acid reflux. Several factors also increase one’s chances of having sleep apnea.
High Altitudes
Living in or traveling to places with high altitudes, may increase an individual’s risk of developing sleep apnea. At higher altitudes, there is less oxygen in the atmosphere. Thus, an individual would have reduced oxygen content in their blood, which would create instability in their breathing. They will likely develop high altitude periodic breathing, which is a breathing pattern characterized by deep and rapid breathing alternating with central sleep apnea.
Thus, it is recommended that individuals travelling to high altitudes (>2500 m, or >8000 ft, above sea level) should ascend slowly and drink sufficient amounts of water (dehydration can contribute to sleep apnea by leading to one sleeping with their mouth open), to help the body adjust to the changes in oxygen content. If possible, one’s sleeping altitude should be as low as possible as well.
I never did test my son for sleep apnea, but I came across the info I am sharing above when I was trying to find a solution for his frequent night waking. Moving from living in the mountains (Boulder, CO), to sea level (Los Angeles, CA), was the most impactful to his sleep. He started sleeping from 8pm-7am most nights within a few weeks of moving to California, when previously he had woken up every 2-3 hours all night long (I had noticed he would only wake once a night whenever we traveled to low altitude places in the past). I recently came across a room oxygenator that may be able to help improve sleep for those that do live at high altitudes. I don’t personally have any experience with this, but will consider trying it if we ever move back to our beloved Boulder, CO. ?
Sleeping Posture
Poor sleeping posture can lead to specific forms of sleep apnea such as OSA. Specifically, there are differences in one’s posture that can make an individual more susceptible to developing OSA. These differences affect the space and shape of certain cranial and facial bones.
For example, those with OSA will have a reduced pharyngeal space — this space exists from the bones of the ear, to the upper cervical region of the spine. The reduced space affects an individual’s breathing capabilities. Additionally, those with OSA may also have hyperextension (or increased extension) of the head and a more anterior (or forward) placement of the head.
While these differences make an individual more susceptible to developing OSA, improving sleeping posture can help prevent sleep apnea. For example, sleeping on one’s back may support proper breathing by preventing the airways from collapsing.
The Sleep Apnea & Hashimoto’s Connection
Over the last few years, three of my clients have presented with adrenal fatigue that just wouldn’t budge! They were struggling with their energy levels, and standard adrenal protocols consisting of adaptogenic herbs, B vitamins, vitamin C, sleeping more, de-stressing — and even adrenal hormones — weren’t helping!
Whenever this happens, I always go back through all of their intake documents and labs to see if anything is missing…
Sure enough, one of the clients had sleep apnea and refused to use her CPAP, one of the treatment devices for sleep apnea. Another client reported that she tended to snore, and the third client had a scalloped tongue, but they hadn’t been tested for sleep apnea. I recommended that the latter two clients get tested.
Over the next six months, the two ladies with suspected sleep apnea were found to have it, and all three clients embarked on treatments for the condition.
They reported that addressing their sleep apnea helped them feel significantly less tired, normalize their adrenal function, and reduce their thyroid antibodies.
Research has linked sleep apnea, an increasingly common cause of sleep deprivation, to Hashimoto’s. I previously mentioned that research suggests that OSA-type sleep apnea is more common in those with Hashimoto’s. Additionally, studies have found that 25-35 percent of people with hypothyroidism also have sleep apnea.
Now the question is… does hypothyroidism cause sleep apnea, or does sleep apnea cause hypothyroidism?
As with most triggers that are known to cause and exacerbate Hashimoto’s, it turns out that sleep apnea and Hashimoto’s are a bit of a vicious cycle situation.
Hypothyroidism may make an individual more susceptible to sleep apnea, as this autoimmune condition is associated with factors such as protein deposition in the upper airway (meaning protein can “stick” to respiratory muscles located in the upper airway — leading one to develop mucus and become weaker), an increased risk of obesity (due to weight gain being a common thyroid symptom), an enlarged tongue (due to swelling), and abnormal control over breathing. All of these factors increase one’s risk of developing sleep apnea. That said, researchers wanted to know if sleep apnea itself could be a potential trigger in Hashimoto’s.
They studied the incidence of thyroid antibodies in people with and without the OSA form of sleep apnea. A 2012 study published in Endocrine Journal showed that 53.2 percent of people with obstructive sleep apnea were positive for thyroid peroxidase (TPO) or thyroglobulin (TG) antibodies, or both, and thus had some stage of Hashimoto’s. (Read more about the 5 stages of Hashimoto’s.)
Some of the people in the study group still had “normal” TSH numbers, so they had not yet developed overt hypothyroidism, suggesting that OSA may be a causative factor for Hashimoto’s.
The researchers concluded that “repetitive episodes of oxygen deprivation followed by reoxygenation result in a generation of reactive oxygen species which can up-regulate inflammatory pathways activating the Th-1 immune pathway which has been implicated in Hashimoto’s.” In other words, long-term obstructive sleep apnea can increase the risk of Hashimoto’s and is an important trigger to consider.
In this same study, researchers learned that the more severe the sleep apnea, the more likely the subjects were to have Hashimoto’s. Here are some other notable findings:
- Males with sleep apnea were especially likely to have Hashimoto’s; 66 percent of men with sleep apnea had Hashimoto’s antibodies!
- People with sleep apnea and Hashimoto’s had a higher number of thyroid antibodies (compared to those with Hashimoto’s who did not have sleep apnea); those with OSA had TGAb in the 1,000 IU/mL range, while people without had TGAb in the 400 IU/mL range.
- People with sleep apnea and Hashimoto’s also had a higher number of TPO antibodies; those with sleep apnea had an average of 4,490 IU/mL compared to those without who had an average of 650 IU/mL.
Testing for Sleep Apnea
If you’re experiencing sleep issues and suspect you may have sleep apnea, your doctor may refer you to a sleep clinic where you may be enrolled in a sleep study. Sleep studies are considered the most reliable testing for sleep apnea and other sleep disorders.
A sleep study involves sleeping at a specialized lab where the person’s vital signs, brain activity, and breathing patterns are recorded and monitored for the following:
- Vital signs — Your heart rate, lung activity, and blood oxygen levels will be monitored by researchers. (Some vitals such as heart rate and respiratory rate can also be self measured by devices such as the Oura ring.) Those with sleep apnea will have higher heart rates, decreased lung volume, increased airflow resistance, and low oxygen levels, as well as more variability in blood pressure.
- Brain activity — Sleep apnea deprives the brain of oxygen. Thus, abnormalities in brain activity, measured by a brain imaging device, may indicate sleep apnea. Abnormalities vary between individuals, but typically reflect disrupted activity due to a loss of white matter (a type of brain tissue) in the brain.
- Breathing patterns — Different breathing patterns may be observed depending on the type of sleep apnea that the individual may experience, such as high altitude-related periodic breathing, as mentioned previously. Generally speaking, an absence of airflow and/or absence of an effort to breathe will be reflected in one’s breathing patterns, if sleep apnea is present.
If you have central sleep apnea, your doctor may refer you to a cardiologist or neurologist for further evaluation. If you have obstructive sleep apnea, your doctor may refer you to an ear, nose, and throat specialist to rule out any airway blockages as a cause.
Conventional Sleep Apnea Protocols
The most well-known treatment for sleep apnea is the continuous positive airway pressure (CPAP) machine, which is used to maintain breathing.
Some also find benefits from using a dental device (known as a mandibular advancement device), which is a type of retainer-like appliance that is worn overnight to gently open airways.
Sometimes, medications may also be prescribed.
CPAP Machines
CPAP stands for “continued positive airway pressure” and is a non-surgical therapy usually used as the first line of treatment for obstructive sleep apnea. It is a small machine that uses mild air pressure in order to keep your airways open while you sleep — the air pressure from the machine is greater than the surrounding air, which keeps your upper airway passages open. It contains a mask that goes over the nose and mouth, so it may take some getting used to! However, it is the chosen treatment for severe cases of sleep apnea for a reason.
When used correctly and consistently, it is extremely effective in cutting down on daytime sleepiness, reducing or eliminating snoring, lessening chances of cardiovascular problems and stroke, and improving cognitive function and memory. As I previously mentioned, treating sleep apnea is an important step in addressing symptoms of Hashimoto’s and hypothyroidism.
Side effects of CPAP usage may include congestion, runny nose, or dry mouth. Furthermore, the mask may be uncomfortable and need adjustments to get the perfect fit. Maintaining cleanliness of the mask and replacing it as recommended, are essential in lessening discomfort. That said, a CPAP machine can be incredibly helpful.
An added benefit to those who have adrenal fatigue, is that use of the CPAP machine has been proven to lower evening cortisol levels. A 2011 study that researched the effect of the CPAP on cortisol levels revealed that just two weeks of CPAP treatment lowered morning cortisol levels. After three months, evening cortisol levels were lowered. This is good news for people who are prone to hyperarousal and lack of replenishing sleep!
It can be deduced that the longer and more consistent the CPAP treatment, the greater the positive effect on the HPA axis. Although I would not recommend running out and getting a CPAP machine without getting a proper sleep apnea diagnosis, it does amplify the many benefits of treating sleep apnea as you work to address the many symptoms of Hashimoto’s.
Mandibular Advancement Therapy
A mandibular advancement device (MAD) moves the lower jaw forward, allowing for a better flow of oxygen to the airway while we sleep. This type of device may be especially helpful for those who have a small or receding jaw, or for those with an enlarged tongue that can block the airway.
Much like a retainer, the mandibular advancement devices work best when they are fitted to your mouth. While the MAD is not as well known as the CPAP, the devices have shown to be equally effective, even in cases of severe sleep apnea.
Although surgery is a second-line therapy for individuals with sleep apnea, one surgical option for individuals who do respond to implementing lifestyle changes or devices such as the CPAP or MAD, is the anterior mandibular osteotomy (bone cutting). The anterior mandibular osteotomy procedure is relatively minimally invasive and has a 67 percent success rate. The main reasons for the failure of this surgical procedure are obesity and abnormal mandibular skeletal structure.
Medications
While conventional doctors may prescribe Valium, nonbenzodiazepine hypnotics such as Ambien, and benzodiazepines (like temazepam) to address a patient’s insomnia, these medications should NOT be used in people with sleep apnea due to their inhibitory effects on the central nervous system. In particular, benzodiazepines should be avoided in people with sleep apnea.
Additionally, there are other medications that may exacerbate OSA and theoretically worsen daytime sleepiness, such as:
- Benzodiazepine receptor agonists
- Barbiturates
- Antiepileptic medications
- Sedating antidepressants such as mirtazapine (antidepressants can cause weight gain, which worsens sleep apnea due to obesity)
- Antihistamines
- Opiates
Various medications have been studied for treating obstructive sleep apnea, including drugs that stimulate the respiratory system (directly like theophylline, or indirectly like acetazolamide), drugs that reduce risk of upper airway collapse (desipramine), antimuscarinic drugs (oxybutynin), and noradrenergic drugs (atomoxetine), but none of them have yet shown a significant ability to reduce OSA. (That said, acetazolamide, a drug used for altitude sickness, can be used to treat and help prevent high altitude periodic breathing in those living at high altitudes.)
One drug in particular, dronabinol, has been shown to significantly reduce one’s apnea-hypopnea index, but did not affect wakefulness in a phase II clinical study — thus, it may not be an effective therapy to address the diverse symptoms observed in sleep apnea.
Due to the limitations of actually helping the sleep apnea, the mainstay of conventional prescription therapy for sleep apnea is focused on addressing one of the most obvious consequences of sleep apnea: excess daytime sleepiness. Although the drugs do not have sufficient evidence to improve OSA itself, modafinil and armodafinil are used to promote daytime wakefulness.
The Root Cause Approach
While the conventional approach can be helpful in addressing sleep apnea, I also recommend digging for additional root causes like food sensitivities, nutrient deficiencies, and infections that could be contributing to symptoms of sleep apnea and Hashimoto’s, and really looking at the body as a whole.
First and foremost, we have to start with nutrition. Eating an anti-inflammatory diet, like the Autoimmune Paleo diet, can help reduce some of the inflammation that may be correlated with sleep apnea (research has found that inflammation can disrupt an optimally functioning circadian rhythm). Furthermore, addressing nutrient deficiencies can improve how we feel, as well as potentially improve our sleep apnea.
While more studies are needed, by looking at root causes, we may see an improvement and resolution of both Hashimoto’s and sleep apnea. I recommend starting with simpler strategies such as dietary interventions and supplements, before considering more advanced strategies such as feedback techniques and sleeping tools.
Dietary Interventions for Sleep Apnea
A 2011 case study report demonstrated that dietary interventions can be an effective tool to improve sleep apnea. In this case study, the authors aimed to improve an individual’s OSA through dietary changes. These changes consisted of the individual following a polymeal diet (a diet aimed at reducing cardiovascular disease risk) that focused on nutrient-dense foods such as high quality animal products (lean meats, omega-3-rich eggs), as well as vegetables and nuts. The consumption of processed foods was limited to a rare occurrence or two. The individual was also encouraged to add spices such as turmeric and garlic when cooking.
The researchers found that following this diet resulted in a complete resolution of the individual’s sleep apnea (and the individual no longer needed his CPAP machine!).
I often recommend that individuals with Hashimoto’s follow a nutrient-dense and thyroid-friendly diet such as the Paleo diet, which is similar to the polymeal diet mentioned in the study above — check out my article on the best diet for Hashimoto’s for more information.
Addressing Nutrient Deficiencies & Mitochondria
In addition to making dietary changes, addressing possible nutrient deficiencies can help improve sleep apnea.
A 2012 case study reported that a 24-year old who received treatment for Leigh disease, a mitochondrial condition that presents with neurological symptoms, had an improvement in not just their Leigh disease symptoms but also in his obstructive sleep apnea, as documented by a sleep study that occurred one year after his initial diagnosis and treatment plan was started.
Interestingly, the recommended treatment for Leigh’s disease consisted of many nutrients that I already recommend for people with Hashimoto’s, that also support the mitochondria, including CoQ10, thiamine, carnitine, vitamin C, and vitamin E.
Research has shown that these nutrients can support mitochondrial function, improve brain function, reduce neurological damage and, in doing so, help support good quality sleep (which means a reduced risk of experiencing sleep apnea).
Vitamin D deficiency can also lead to OSA, as low levels of this vitamin are associated with increased inflammation and poor immune function (which contribute to sleep issues such as sleep apnea). This deficiency is commonly observed in those with Hashimoto’s — research has found that individuals with Hashimoto’s have significantly lower levels of vitamin D. In my survey of over 2000 individuals with Hashimoto’s, 68 percent of individuals said they had low vitamin D levels.
Thiamine is another common nutrient depletion seen in people with Hashimoto’s and has been a life-changing nutrient for many. There may be some evidence of this nutrient playing an important role in central sleep apnea, as well as obstructive sleep apnea.
Read more about addressing vitamin D and thiamine depletions in the section below.
Supplements To Consider With Sleep Apnea
Various supplements may be helpful for addressing sleep apnea. Some of them have promising (albeit small) studies supporting their efficacy in reducing obstructive, central and mixed apnea types directly. Other supplements may be helpful through targeting overall inflammation. Additionally, some supplements address the consequences of sleep apnea.
Let’s start with the five most relevant ones that may help with reducing sleep apnea:
- Thiamine — Thiamine (B1) can be especially helpful for central sleep apnea, as it supports brain and mitochondrial health. As mentioned previously, decreases in the brain’s oxygen levels can make an individual more susceptible to developing sleep apnea. By supporting the brain while oxygen levels fluctuate, thiamine can help ensure brain function is optimal, and that the brain and muscles required for breathing during sleep are communicating properly. The supplement I have taken is the highly absorbable BenfoMax by Pure Encapsulations. I recommend 600 mg per day for most people as a starting point.
- NAC — N-acetyl cysteine, or NAC, is well known for its role in liver health. But did you know that it can also help sleep apnea? The available research also suggests that long-term treatment of sleep apnea with NAC can reduce an individual’s dependency on CPAP. Additionally, one study found that NAC can significantly improve sleep apnea by increasing glutathione production and reducing lipid peroxidation (a physiological process that results in oxidative stress). Glutathione is a potent antioxidant that can repair liver damage caused by sleep apnea. Interestingly, low levels of this antioxidant have been linked to sleep apnea. The precursor to glutathione, cysteine, can provide additional support by reducing snore time and duration. To benefit from these three nutrients, I recommend Rootcology’s Pure N-Acetyl Cysteine at a daily dose of 1800 mg per day.
- CoQ10 — This antioxidant supports the mitochondria (involved in oxygen delivery and breathing, both of which are implicated in sleep apnea), as well as helps reduce inflammation, thus improving sleep quality and reducing sleep apnea. I recommend taking 200-500 mg per day of CoQ10.
- Omega-3s — Similarly to CoQ10, omega-3 fatty acids reduce inflammation, which can improve sleep quality. As mentioned previously, research has found that supplementing with omega-3s (or eating adequate amounts of omega-3-rich foods) can improve (and in some cases, even eliminate) sleep apnea. To get enough omega-3 fatty acids, I recommend a professional quality fish oil supplement that has been molecularly distilled and filtered, such as EPA/DHA Essentials by Pure Encapsulations or OmegAvail™ Synergy by Designs for Health. Omega-3s can also help with brain repair after OSA-related hypoxic injury.
- Progesterone — While this hormone is heavily involved in fertility and menstrual health, it actually plays a wide variety of roles. One of the lesser mentioned roles of progesterone is in sleep quality. Progesterone helps induce sleep and promotes healthy respiration during sleep. Research has found that progesterone reduces both obstructive and central sleep apnea in men. Studies have also shown that progesterone can reduce apnea in menopausal women with obesity hypoventilation syndrome. Oral progesterone can work quickly — however, the dosage will be unique for each individual. I recommend starting on a low dose (12.5 mg slow release at bedtime) and observing whether that helps. While there are some topical progesterone options available as supplements, oral progesterone is a prescription drug. As with all hormones, I always recommend working with your healthcare practitioner to determine your ideal dosage. Interestingly, progesterone deficiency/estrogen dominance is a common pattern I see in Hashimoto’s as well.
In addition to the five relevant supplements mentioned above, there are some additional supplements that have been shown to improve sleep apnea and sleep quality:
- Vitamin D — Studies have found that vitamin D deficiency is common in both those with Hashimoto’s, and those with sleep apnea. While the role of vitamin D in sleep apnea is complex and still not completely understood, researchers hypothesize that vitamin D deficiency can lead to weakness of muscles surrounding the mouth, making an individual more susceptible to obstruction. To ensure you have adequate levels of vitamin D, I recommend supplementing with vitamin D3 at a starting dose of around 5000 IU per day. I recommend either Pure Encapsulations Vitamin D3 (does not contain vitamin K) or Designs for Health Vitamin D Supreme (contains vitamin K for those who are deficient in it, as supplementing with only vitamin D when one is deficient in vitamin K, can have a negative impact on the arteries).
- Probiotics — Probiotics support healthy gut function by providing “good” bacteria to balance out pathogenic strains. Given that the majority of our immune cells reside in our gut, a healthy gut encourages a healthy immune function and reduces inflammation. As mentioned previously, inflammation disrupts the functioning of the circadian rhythm. Animal studies have shown that probiotics reduce systemic inflammation as well as hypoxia (a condition where not enough oxygen makes it to the tissues and cells in the body, contributing to sleep apnea). As such, probiotics can encourage good quality sleep and reduce one’s risk of sleep apnea.
- Selenium — Research has shown that selenium can help reduce snoring seen in sleep apnea (especially non-obesity-related sleep apnea), which may help in regulating breathing patterns and ensuring enough oxygen is getting to the cells. For most people, I recommend Selenium from Pure Encapsulations, at a dose of 200 mcg per day. It will typically take 3-5 days for symptoms to show improvement.
- Fulvic acid — Fulvic acid is a naturally occurring compound found in water and soils, formed when living things decompose. This substance is often extracted from shilajit (a sticky substance primarily found in the rocks of the Himalayas, that is rich in fulvic acid) for its immune-boosting properties. Interestingly, it has been shown to improve sleep quality and may also help with issues related to high altitude. Fulvic acid and shilajit can be consumed as a supplement.
Supplements That May Reduce Sleep Apnea-Related Complications
Because sleep apnea interferes with our ability to get proper rest and leads to mini-hypoxic events in the brain and body (when they are deprived of oxygen), this can lead to numerous health complications. When our cells don’t have enough oxygen (this is called hypoxia), symptoms such as shortness of breath, headaches (and, in severe cases, cognitive and heart issues) can develop.
Hypoxia can also lead to suboptimal liver function and oxidative stress (physical stress from high levels of harmful, oxygen-based molecules).
Additionally, several nutrient depletions such as deficiencies in vitamins A and D, as well as in glutathione, are all often seen in individuals who experience sleep apnea.
The following supplements can help address these complications:
- Vitamin E and C — Both vitamin E and C work synergistically (meaning their combined benefits are greater than the benefits of one of these alone) to improve oxidative stress seen in sleep apnea. Vitamin C also improves the health of blood vessels (which are impacted due to getting lower oxygen). For vitamin E, I recommend Integrative Therapeutics Vitamin E, which is a professional, high-quality brand that includes 400 IU of vitamin E (as d-alpha tocopherol), plus 50 mg mixed tocopherols (gamma, delta, alpha, and beta). NOW Sun-E 400 also offers a soy-free, natural vitamin E, which is derived from non-GMO sunflower seed oil. It contains 400 IU of vitamin E (as D-Alpha tocopherol). For vitamin C, I recommend experimenting with supplementing between 500 and 2000 mg per day, or as recommended by your provider. I like NOW Brand’s Vitamin C-500.
- Vitamin A — Individuals with sleep apnea have been shown to have low amounts of vitamin A, and low levels of this vitamin have been linked to cardiovascular complications. Thus, supplementing with vitamin A can promote cardiovascular health by encouraging healthy function of blood vessels.
- Other B vitamins — Other B vitamins, such as vitamins B6, B9 (folate), and B12, can reduce hypoxia and support healthy brain function. B Complex Plus by Pure Encapsulations is a great option, as it contains all the aforementioned B vitamins. Additionally, choline can work with B vitamins to further reduce hypoxia. I recommend Vital Nutrients Citicoline at a dose of 500-2000 mg/day.
- Copper — Copper levels are a strong predictor of how much oxidative stress is present within those who have sleep apnea — low copper levels are associated with more oxidative stress. Increasing copper intake can help fight harmful free radicals and improve oxidative damage. That said, I always recommend ruling out copper toxicity, before supplementing with copper, and also making sure you are getting adequate amounts of zinc (max 30 mg per day).
- Magnesium, manganese, and zinc — Supplementing with minerals such as magnesium, manganese and zinc (along with selenium, as mentioned previously) can help improve damage caused by hypoxia in those who have sleep apnea. I recommend the zinc picolinate version (I usually recommend doses of no more than 30 mg per day), such as the one made by Pure Encapsulations, because of its improved absorption profile compared to other forms. For magnesium supplementation, I recommend Magnesium Citrate Powder by Rootcology for people with Hashimoto’s and constipation. For those with diarrhea and Hashimoto’s, I recommend Magnesium Glycinate by Pure Encapsulations. For manganese, I recommend Manganese by Pure Encapsulations, 5-15 mg per day.
Underlying Infections That May Contribute to Sleep Disturbances
Infections (such as upper respiratory tract infections) can lead to sleep apnea, as they result in inflammation or swelling of the airway and nasal passages. Such blockages can then lead to improper breathing during sleep (leading to sleep apnea).
Two common infections that may be Hashimoto’s triggers and can also contribute to sleep apnea, include Streptococcus pyogenes (the bacteria that causes “strep throat”), as well as the Epstein-Barr virus (EBV). Both can cause enlarged tonsils, which can lead to a blockage of airway passages.
Streptococcus pyogenes
One study found a significant association between obstructive sleep apnea and Streptococcus pyogenes. The authors described that this pathogen releases toxins within the tonsils, causing them to be swollen and enlarged, allowing for obstructive sleep apnea to develop.
The authors found infections from other pathogens such as H. influenzae and S. pneumoniae to also be significantly associated with the development of obstructive sleep apnea.
Interestingly, there is an association between infections, tonsillectomies (the removal of tonsils), and the development of thyroid disease.
Many years ago, tonsillectomies were a common recommendation for individuals who experienced recurrent tonsillitis (or infections of the tonsils) due to infections such as strep throat. It is also becoming more common to recommend tonsillectomies to those who have developed obstructive sleep apnea. Some physicians report that individuals who have had tonsillectomies to resolve such infections, experience an improvement in sleep apnea, and others in their thyroid symptoms.
However, the tonsils act as a protective barrier to the thyroid (they share similar blood supplies), and some integrative practitioners believe that tonsillectomies should be avoided, as they act to filter out toxins that would otherwise impact the rest of the body. Interestingly, research shows individuals who have tonsillectomies are at higher risk of developing malignant (or lethal) thyroid cancer at a younger age.
As for the link between these infections and thyroid disease, I am beginning to believe Streptococcus pyogenes is a common trigger for Hashimoto’s. I’ve realized that overgrowth of this strep pathogen is a very common bacterial dysbiosis pattern on stool tests. In my recent survey of clients who took the GI-MAP test, 58 percent of samples had Streptococcus, although only 25 percent of these were flagged as having abnormal levels per lab standards.
One study showed that a Streptococcal infection can trigger a thyroid storm (a life-threatening condition), in which low TSH and high T3 and T4 are observed.
If you have a history of recurrent strep throat infections, you may want to consider a probiotic with a beneficial strain of Streptococcal bacteria that can crowd out the potentially pathogenic kind. One specific beneficial strain of S. salivarius called K12, has been found in individuals who show a natural resistance to Streptococcus pyogenes. It contains “lantibiotics” that inhibit many strains of Streptococcus pyogenes and can help prevent strep throat. This is something I learned about from my son’s pediatrician and have recommended to clients.
I have not done a retroactive case review to see how many clients reported to have recurrent strep throats before their Hashimoto’s diagnosis, but I do remember this coming up numerous times. I personally had recurring strep throat and EBV in college, and this led me to develop hypersomnia, and later, Hashimoto’s. I was not tested for sleep apnea at that time, but I do remember feeling self-conscious about my scalloped tongue back then.
Epstein-Barr Virus (EBV)
I have found EBV (which you may have heard of if you’re familiar with “mono”, or the mononucleosis infection) to be common in those with Hashimoto’s. A 2015 Polish study found EBV in the thyroid cells of 80 percent of people with Hashimoto’s, and 62.5 percent of people with Graves’, while controls did not have EBV present in their thyroid gland. Furthermore, cells suggesting a continually proliferating state — a slowly growing infection — were found in the Hashimoto’s group as well.
In children, EBV does not usually cause symptoms (it is asymptomatic). In teens and young adults, the virus is symptomatic only 50 percent of the time. When it is symptomatic, the most common symptoms include fatigue, hypersomnia, sore throat, and swollen lymph nodes. Weight loss is also common. EBV can significantly increase the size of lymphoid tissue (involved in the immune system) when there is an infection.
In a person with poor nutrition and vulnerabilities, the virus may defeat and deplete the body’s immune response, resulting in a low-grade latent infection, as well as multiple deficiencies and imbalances that pave the way for the autoimmune process to take hold… leading to the symptoms mentioned above.
Moreover, specific immune cells known as CD8+ T cells, are needed to fight off the Epstein-Barr virus. However, some individuals may have a low baseline level of these types of immune cells. CD8+ T cells decrease with age, are lower in women, and are also decreased when vitamin D intake is low. When levels of these fighter cells are insufficient, the Epstein-Barr virus may take up residence in our organs (such as the thyroid) and essentially hijack the organ to help the virus hide and multiply.
While EBV is usually self-resolving, meaning it usually resolves on its own, in some individuals this virus can become latent and lead to other conditions such as Hashimoto’s.
It is also correlated with obstructive sleep apnea (OSA). One case study reported an individual developed obstructive sleep apnea after being infected with EBV. A common complication of this virus is that, like Streptococcus pyogenes, it leads to enlarged tonsils, which then causes airway obstruction. Research suggests that this may be the method behind how EBV can lead to obstructive sleep apnea. While this is mostly reported in acute cases of EBV, I often wonder if chronic EBV conditions can lead to sleep apnea as well.
I don’t think there are specific studies of sleep apnea induced by chronic EBV, but if you follow the trail, you will see that many of the disorders that can be triggered by EBV, such as chronic fatigue syndrome and Hashimoto’s, tend to have high rates of sleep apnea.
Furthermore, cases of chronic fatigue post-EBV have been associated with symptoms that are commonly seen in individuals with sleep apnea, such as daytime sleepiness or idiopathic hypersomnia.
You can do testing to determine if an EBV infection could be a root cause of your sleep apnea (and autoimmune thyroid condition), and read more about Epstein-Barr virus in this article.
I also have more information about root cause testing, including a questionnaire to help you prioritize which ones to address first, in the Advanced Protocols chapter of my book Hashimoto’s Protocol.
Advanced Strategies to Reduce Sleep Apnea
If you are still struggling with sleep apnea after trying the recommendations above, consider looking into some advanced strategies.
Feedback Techniques: Biofeedback and Neurofeedback
Biofeedback and neurofeedback may be effective methods of improving sleep apnea.
With biofeedback, physiological processes are monitored with sensors, and the body is given “feedback” to help regulate these processes.
Neurofeedback involves using a brain activity-monitoring device called an electroencephalography (EEG) to measure brain activity. The EEG procedure involves a physician or neurologist placing electrodes on different parts of the scalp which correspond to different parts of the brain.
Data about brain activity is then extracted and read as either positive or negative feedback. As the individual receives the feedback, they will alter their actions towards the desired brain activity.
The idea here is that the brain and body “learn” how to better regulate certain functions together.
In the case of sleep apnea, both these feedback techniques can help to “train” the body and brain towards better sleep function. Training may involve helping to strengthen the connection between the brain and breathing muscles, or promoting sleep-inducing brain activity, depending on each individual’s needs.
Research has shown that biofeedback is a promising therapy for improving adult sleep conditions such as sleep apnea. Neurofeedback with EEG has been successfully used to treat sleep apnea in males. One study found that using neurofeedback also improves sleep apnea, as evidenced by a reduction in brain wave activity that is associated with sleep apnea.
Takeaway
Sleep apnea is a condition that has been linked to Hashimoto’s, and many individuals with Hashimoto’s who also experience sleep apnea feel worse due to the sleep deprivation and adrenal fatigue that this condition creates.
From a root cause approach, factors such as nutrient deficiencies and infections can lead to sleep apnea. However, addressing these issues as well as considering supplements such as progesterone, shilajit/fulvic acid, and/or valerian can improve sleep quality. Newer technologies such as neurofeedback and biofeedback can also help reduce sleep apnea and lead to better sleep!
Do you have a scalloped tongue? Have you considered sleep apnea as a possible root cause, and have you been tested for it? Because it is so prevalent among those with Hashimoto’s, I recommend that you get tested for sleep apnea, especially if you snore or have a scalloped tongue.
If you have been tested for sleep apnea, I would love to hear from you! What has worked for you to address sleep apnea? Please leave a comment below!
P.S. If you’re interested in improving the quality of your sleep, I recommend reading my article on sleep solutions for Hashimoto’s.
P.P.S. To discover additional root causes that may be at play behind your Hashimoto’s, pick up a copy of Hashimoto’s Protocol: A 90-Day Plan for Reversing Thyroid Symptoms and Getting Your Life Back and Hashimoto’s Thyroiditis: Lifestyle Interventions for Finding and Treating the Root Cause.
You can also download a Thyroid Diet Guide, 10 thyroid-friendly recipes, and the Nutrient Depletions and Digestion chapter of my first book for free! You will also receive occasional updates about new research, resources, giveaways and helpful information.
For future updates, make sure to follow me on Facebook and Instagram, too!
References
- Bozkurt N, Karbek B, Cakal E, Firat H, Ozbek M, Delibasi T. The association between severity of obstructive sleep apnea and prevalence of Hashimoto’s Thyroiditis. Endocrine Journal. 2012;59(11):981-988. doi:10.1507/endocrj.ej12-0106.
- Magrini A, Pietroiusti A, Coppeta L et al. Shift Work and Autoimmune Thyroid Disorders. International Journal of Immunopathology and Pharmacology. 2006;19(4):31-35.
- Bozkurt NC, Karbek B, Cakal E, Firat H, Ozbek M, Delibasi T. The association between severity of obstructive sleep apnea and prevalence of Hashimoto’s thyroiditis. Endocr J. 2012;59(11):981-988. doi:10.1507/endocrj.ej12-0106
- Fisher S, Lewis KE, Bartle I, Ghosal R, Davies L, Blagrove M. Emotional content of dreams in obstructive sleep apnea hypopnea syndrome patients and sleepy snorers attending a sleep-disordered breathing clinic. J Clin Sleep Med. 2011;7(1):69-74.
- Harper RM, Kumar R, Ogren JA, Macey PM. Sleep-disordered breathing: effects on brain structure and function. Respir Physiol Neurobiol. 2013;188(3):383-391. doi:10.1016/j.resp.2013.04.021
- Mermigkis C, Bouloukaki I, Mastorodemos V et al. Medical treatment with thiamine, coenzyme Q, vitamins E and C, and carnitine improved obstructive sleep apnea in an adult case of Leigh disease. Sleep and Breathing. 2013;17(4):1129-1135. doi:10.1007/s11325-013-0816-5.
- Mete T, Yalcin Y, Berker D et al. Relationship between obstructive sleep apnea syndrome and thyroid diseases. Endocrine. 2013;44(3):723-728. doi:10.1007/s12020-013-9927-9.
- Chandna S, Bathla M. Oral manifestations of thyroid disorders and its management. Indian J Endocrinol Metab. 2011;15(Suppl 2):S113-S116. doi:10.4103/2230-8210.83343
- Fukusumi M, Iidaka T, Mouri A, Hamamoto Y, Kamimura M. Respiratory failure associated with hypoventilation in a patient with severe hypothyroidism. Respirol Case Rep. 2014;2(2):79-80. doi:10.1002/rcr2.55
- Hashimoto’s disease. Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/hashimotos-disease/symptoms-causes/syc-20351855. Published February 11, 2020. Accessed August 20, 2021.
- Wiersinga WM. Adult hypothyroidism. Endotext [Internet]. https://www.ncbi.nlm.nih.gov/books/NBK285561/. Published March 28, 2014. Accessed August 20, 2021.
- Kapur VK, Koepsell TD, deMaine J, Hert R, Sandblom RE, Psaty BM. Association of hypothyroidism and obstructive sleep apnea. Am J Respir Crit Care Med. 1998;158(5 Pt 1):1379-1383. doi:10.1164/ajrccm.158.5.9712069
- Raff H, Ettema S, Eastwood D, Woodson B. Salivary Cortisol in Obstructive Sleep Apnea: The Effect of CPAP. Endocrine. 2011;40(1):137-139. doi:10.1007/s12020-011-9474-1.
- Piccin CF, Pozzebon D, Scapini F, Corrêa EC. Craniocervical Posture in Patients with Obstructive Sleep Apnea. Int Arch Otorhinolaryngol. 2016;20(3):189-195. doi:10.1055/s-0036-1584295
- Serra-Torres S, Bellot-Arcís C, Montiel-Company J, Marco-Algarra J, Almerich-Silla J. Effectiveness of mandibular advancement appliances in treating obstructive sleep apnea syndrome: A systematic review. The Laryngoscope. 2015;126(2):507-514. doi:10.1002/lary.25505.
- Weiss T. Association of tongue scalloping with obstructive sleep apnea and related sleep pathology. Otolaryngology – Head and Neck Surgery. 2003;129(2):P179-P180. doi:10.1016/s0194-5998(03)01047-7.
- White D, Shafazand S. Mandibular Advancement Device vs CPAP in the Treatment of Obstructive Sleep Apnea: Are they Equally Effective in Short Term Health Outcomes?. Journal of Clinical Sleep Medicine. 2013. doi:10.5664/jcsm.3008.
- Mehra P, Wolford LM. Surgical management of obstructive sleep apnea. Proc (Bayl Univ Med Cent). 2000;13(4):338-342. doi:10.1080/08998280.2000.11927701
- Weaver E, Kapur V. Surgical Treatment of Obstructive Sleep Apnea in Adults. UpToDate. https://www.uptodate.com/contents/surgical-treatment-of-obstructive-sleep-apnea-in-adults. Accessed December 10, 2021.
- Kryger M, Malhotra A. Management of Obstructive Sleep Apnea in Adults. UpToDate. https://www.uptodate.com/contents/management-of-obstructive-sleep-apnea-in-adults?search=sleep+apnea+medication&source=search_result&selectedTitle=1~150&usage_type=default&display_rank=1. Accessed December 10, 2021.
- Alzoubi MR, Aldomi Al-Domi H. Could omega-3 fatty acids a therapeutic treatment of the immune-metabolic consequence of intermittent hypoxia in obstructive sleep apnea?. Diabetes Metab Syndr. 2017;11(4):297-304. doi:10.1016/j.dsx.2016.06.024
- Andersen ML, Bittencourt LR, Antunes IB, Tufik S. Effects of progesterone on sleep: a possible pharmacological treatment for sleep-breathing disorders?. Curr Med Chem. 2006;13(29):3575-3582. doi:10.2174/092986706779026200
- Carrasco-Gallardo C, Guzmán L, Maccioni RB. Shilajit: a natural phytocomplex with potential procognitive activity. Int J Alzheimers Dis. 2012;2012:674142. doi:10.1155/2012/674142
- Schepetkin IA, Xie G, Jutila MA, Quinn MT. Complement-fixing activity of fulvic acid from Shilajit and other natural sources. Phytother Res. 2009;23(3):373-384. doi:10.1002/ptr.2635
- Shinjyo N, Waddell G, Green J. Valerian Root in Treating Sleep Problems and Associated Disorders-A Systematic Review and Meta-Analysis. J Evid Based Integr Med. 2020;25:2515690X20967323. doi:10.1177/2515690X20967323
- Gala TR, Seaman DR. Lifestyle modifications and the resolution of obstructive sleep apnea syndrome: a case report. J Chiropr Med. 2011;10(2):118-125. doi:10.1016/j.jcm.2010.12.003
- Archontogeorgis K, Nena E, Papanas N, Steiropoulos P. The role of vitamin D in obstructive sleep apnoea syndrome. Breathe (Sheff). 2018;14(3):206-215. doi:10.1183/20734735.000618
- Progesterone for sleep? Progesterone, Insomnia, Oral Progesterone and Insomnia – Compound Pharmaceutical Technologies. https://www.cptinc.org/more-info/progesterone-for-sleep. Accessed July 20, 2021.
- Marzbani H, Marateb HR, Mansourian M. Neurofeedback: A Comprehensive Review on System Design, Methodology and Clinical Applications. Basic Clin Neurosci. 2016;7(2):143-158. doi:10.15412/J.BCN.03070208
- Marzbani H, Marateb HR, Mansourian M. Neurofeedback: A Comprehensive Review on System Design, Methodology and Clinical Applications. Basic Clin Neurosci. 2016;7(2):143-158. doi:10.15412/J.BCN.03070208
- Lacedonia D, Carpagnano GE, Crisetti E, et al. Mitochondrial DNA alteration in obstructive sleep apnea. Respir Res. 2015;16(1):47. Published 2015 Apr 7. doi:10.1186/s12931-015-0205-7
- Yu L, Chen Y, Wang W, Xiao Z, Hong Y. Multi-Vitamin B Supplementation Reverses Hypoxia-Induced Tau Hyperphosphorylation and Improves Memory Function in Adult Mice. J Alzheimers Dis. 2016;54(1):297-306. doi:10.3233/JAD-160329
- Busko M. Shrunken brain structures in sleep apnea. Medscape. https://www.medscape.com/viewarticle/576043. Published July 26, 2020. Accessed July 26, 2021.
- Sleep apnea linked to memory loss. MedicineNet. https://www.medicinenet.com/script/main/art.asp?articlekey=90191. Published June 12, 2008. Accessed July 26, 2021.
- Inflammation can lead to circadian sleep disorders: Novel technology turns inflammation on and off, affecting body clock in mice. ScienceDaily. www.sciencedaily.com/releases/2018/10/181031124858.html. Published October 31, 2018. Accessed August 4, 2021.
- Ucan B, Sahin M, Sayki Arslan M, et al. Vitamin D Treatment in Patients with Hashimoto’s Thyroiditis may Decrease the Development of Hypothyroidism. Int J Vitam Nutr Res. 2016;86(1-2):9-17. doi:10.1024/0300-9831/a000269
- Sandhaus S. Sleep apnea. Sleep Apnea – Life Extension. https://www.lifeextension.com/protocols/respiratory/sleep-apnea. Accessed July 26, 2021.
- Sadasivam K, Patial K, Vijayan VK, Ravi K. Anti-oxidant treatment in obstructive sleep apnoea syndrome. Indian J Chest Dis Allied Sci. 2011;53(3):153-162.
- Sadasivam K, Patial K, Vijayan V et al. Anti-oxidant treatment in obstructive sleep apnoea syndrome. Indian J Chest Dis Allied Sci. 2011;53:153-162.
- Liu J, Zhang J, Lu G et al. The effect of oxidative stress in myocardial cell injury in mice exposed to chronic intermittent hypoxia. Chin Med J. 2010;123:74-78.
- Sekhar R, Patel S, Guthikonda A et al. Deficient synthesis of glutathione underlies oxidative stress in aging and can be corrected by dietary cysteine and glycine supplementation. Am J Clin Nutr. 2011;94:847-853.
- Dunleavy M, Bradford A, O’Halloran K. Oxidative stress impairs upper airway muscle endurance in an animal model of sleep-disordered breathing. Adv Exp Med Biol. 2008;605:458-462.
- Lee D, Badr M, Mateika J et al. Progressive augmentation and ventilatory long-term facilitation are enhanced in sleep apnoea patients and are mitigated by antioxidant administration. J Physiol. 2009;587:5451-5467.
- Murri M, Garcia-Delgado R, Alcázar-Ramirez J et al. Assessment of cellular and plasma oxidative stress in SAHS patients before and after continuous positive airway pressure treatment. Clin Lab. 2010;56:397-406.
- Baldwin C, Bootzin R, Schwenke D et al. Antioxidant nutrient intake and supplements as potential moderators of cognitive decline and cardiovascular disease in obstructive sleep apnea. Sleep Med Rev. 2005;9:459-476.
- Katsoulis K, Kontakiotis T, Spanogiannis D et al. Total antioxidant status in patients with obstruc- tive sleep apnea without comorbidities: the role of the severity of the disease. Sleep Breath. 2011 Dec;15:861-866.
- Grebe M, Eisele HJ, Weissmann N et al. Antioxidant vitamin C improves endothelial function in obstructive sleep apnea. Am J Respir Crit Care Med. 2006;173:897-901.
- Büchner NJ, Quack I, Woznowski M et al. Microvascular endothelial dysfunction in obstructive sleep apnea is caused by oxidative stress and improved by continuous positive airway pressure therapy. Respiration. 2011;82:409-417.
- Celec P, Jurkovičová I, Buchta R et al. Antioxidant vitamins prevent oxidative and carbonyl stress in an animal model of obstructive sleep apnea. Sleep Breath. 2012 June 7 [Epub ahead of print].
- Singh T, Patial K, Vijayan K et al. Oxidative stress and obstructive sleep apnoea syndrome. Indian J Chest Dis Allied Sci. 2009;51:217-224.
- Day R, Matus I, Suzuki Y et al. Plasma levels of retinoids, carotenoids and tocopherols in patients with mild obstructive sleep apnoea Respirology. 2009;14:1134-1142.
- Barcelo A, Barbe F, de la Pena M et al. Antioxidant status in patients with sleep apnoea and impact of continuous positive airway pressure treatment. Eur Respir J 2006;27:756-760.
- Mete T, Yalcin Y, Berker D et al. Obstructive sleep apnea syndrome and its association with vitamin D deficiency. J Endocrinol Invest. 2013 April [Epub ahead of print].
- Bozkurt NC, Cakal E, Sahin M et al. The relation of serum 25-hydroxyvitamin-D levels with severity of obstructive sleep apnea and glucose metabolism abnormalities. Endocrine. 2012;41:518-525.
- Barceló A, Esquinas C, Piérola J et al. Vitamin D Status and Parathyroid Hormone Levels in Patients with Obstructive Sleep Apnea. Respiration. 2012 Nov 15. [Epub ahead of print]
- Dekok H. Case report: the medical treatment of obstructive sleep apnoea syndrome (OSAS) with Selenium. Med Hypotheses. 2005;65:817-818.
- Kato M, Roberts-Thomson P, Phillips B et al. Impairment of endothelium-dependent vasodila- tion of resistance vessels in patients with obstructive sleep apnea. Circulation. 2000;102:2607- 2610.
- Schnabel R, Lubos E, Messow C et al. Selenium supplementation improves antioxidant capacity in vitro and in vivo in patients with coronary artery disease The Selenium Therapy in Coronary Artery disease Patients (SETCAP) Study. Am J Heart. 2008;156:1201e1-11.
- Volná J, Kemlink D, Kalousová M et al. Biochemical oxidative stress-related markers in pa- tients with obstructive sleep apnea. Med Sci Monit. 2011;17:CR491-7.
- Wysocka E, Cofta S, Piorunek T et al. Blood antioxidant status, dysglycemia and obstructive sleep apnea. Adv Exp Med Biol. 2013;756:121-129.
- Wysocka E, Cofta S, Cymerys M et al. The impact of the sleep apnea syndrome on oxidant- antioxidant balance in the blood of overweight and obese patients. J Physiol Pharmacol. 2008;59 Suppl 6:761-769.
- Shan X, Chi L, Ke Y et al. Manganese superoxide dismutase protects mouse cortical neurons from chronic intermittent hypoxia-mediated oxidative damage. Neurobiol Dis. 2007;28:206-215.
- Rosa DP, Martinez D, Picada J et al. Hepatic oxidative stress in an animal model of sleep apnoea: effects of different duration of exposure. Comp Hepatol. 2011;10:1.
- Ntalapascha M, Makris D, Kyparos A et al. Oxidative stress in patients with obstructive sleep apnea syndrome. Sleep Breath. 2012 [Epub ahead of print]
- Mancuso M, Bonanni E, LoGerfo A et al. Oxidative stress biomarkers in patients with un- treated obstructive sleep apnea syndrome. Sleep Med. 2012;13:632-636.
- Martínez-García MÁ, Chiner E. Sleep apnoea and risk of post-operative infection: Beyond cardiovascular impact. European Respiratory Society. https://erj.ersjournals.com/content/49/4/1700292. Published April 1, 2017. Accessed July 26, 2021.
- Millman RP, Bevilacqua J, Peterson DD, Pack AI. Central sleep apnea in hypothyroidism. Am Rev Respir Dis. 1983;127(4):504-507. doi:10.1164/arrd.1983.127.4.504
- Gay PC. Complex sleep apnea: it really is a disease. J Clin Sleep Med. 2008;4(5):403-405.
- Viciani E, Montagnani F, Tavarini S, et al. Paediatric obstructive sleep apnoea syndrome (OSAS) is associated with tonsil colonisation by Streptococcus pyogenes. Sci Rep. 2016;6:20609. Published 2016 Feb 10. doi:10.1038/srep20609
- Raso AM, Dorigo M, Terrando R. Analisi statistica sulle correlazioni tra tonsillectomia e neoplasie maligne della tiroide [Statistical analysis of correlations between tonsillectomy and malignant neoplasms of the thyroid]. Minerva Chir. 1975;30(22):1135-1139.
- Hakoshima M, Yanai H, Komatsuzaki S, Kawaguchi A, Hamasaki H, Katsuyama H. Streptococcal Infection Can Be the Trigger for Thyroid Storm. J Clin Med Res. 2019;11(5):383-384. doi:10.14740/jocmr3818
- Bozkurt NC, Karbek B, Cakal E, Firat H, Ozbek M, Delibasi T. The association between severity of obstructive sleep apnea and prevalence of Hashimoto’s thyroiditis. Endocr J. 2012;59(11):981-988. doi:10.1507/endocrj.ej12-0106
- Cheng J. Obstructive sleep apnea (OSA): a complication of acute infectious mononucleosis infection in a child. Int J Pediatr Otorhinolaryngol. 2014;78(3):561-562. doi:10.1016/j.ijporl.2013.12.029
- Lloyd AM, Reilly BK. Infectious Mononucleosis and Upper Airway Obstruction: Intracapsular Tonsillectomy and Adenoidectomy With Microdebrider for Prompt Relief. Ear Nose Throat J. 2021;100(10_suppl):958S-960S. doi:10.1177/0145561320930046
- Ezreich L. A novel probiotic to reduce the risk of strep throat. Probiotic To Reduce Risk Of Strep Throat – Life Extension. https://www.lifeextension.com/magazine/2015/12/a-novel-probiotic-to-reduce-the-risk-of-strep-throat. Published December 1, 2019. Accessed February 4, 2022.
- Sforza E, Hupin D, Roche F. Mononucleosis: A Possible Cause of Idiopathic Hypersomnia. Front Neurol. 2018;9:922. Published 2018 Oct 31. doi:10.3389/fneur.2018.00922
- Janegova A, Janega P, Rychly B, Kuracinova K, Babal P. Rola infekcji wirusem Epstein-Barr’a w rozwoju autoimmunologicznych chorób tarczycy. Endokrynologia Polska. 2015;66(2):132-136. doi:10.5603/ep.2015.0020.
- Pugliese AF. Sleep apnea: A Case Sleeping Beauty. The ID Doc. https://www.theiddoc.com/sleep-apnea-sleeping-beauty/. Published November 2, 2018. Accessed February 7, 2022.
Note: Originally published in July 2017, this article has been revised and updated for accuracy and thoroughness.